
[ Lay Language Paper Index | Press Room ]
George Lewis, Jr. george@cornellbme.com
William Olbricht
Cornell University,
Ithaca, NY 14850
George Lewis, Sr. thearrayman@transducerengineering.com
Transducer Engineering, Inc.,
Andover, MA 01810
Popular Version of Paper 3aBB5
Presented 9:15 a.m. Thursday, November 29, 2007
154th ASA Meeting, New Orleans, LA
Cornell University scientists in the Department of Biomedical Engineering recently discovered the use of therapeutic ultrasound techniques to enhance drug delivery to neurological tissues in the brain. This breakthrough research in acoustic imaging holds a possible key to increasing the effectiveness of brain cancer treatments, which frequently are ineffective and result in a poor prognosis for people with brain cancer. The scientists believe that combining therapeutic ultrasound treatments with traditional chemotherapy may allow physicians to selectively target malignant tissues with chemotherapy in hard-to-reach areas of the brain that otherwise could not be treated.
Ultrasonic imaging was introduced by Austrian scientist, Karl Theo Dussik in 1942, and continues to be one of the most reliable, safe and simple imaging techniques used routinely by physicians for abdominal, heart, obstetric, vascular, and thyroid imaging. Medical ultrasound imaging systems employ low-power, high frequency sound waves to provide non-invasive images of organs and bodily tissues. The attenuation and reflections of the sound wave traveling through the body and bouncing off various organs and tissues are used to reconstruct the image that is displayed on a monitor. At greater intensities, ultrasound is used as a surgical tool to break up and liquefy bodily tissues. The first study to show the biological effects of “focused ultrasound” was conducted in 1926; by the 1970s focused ultrasound and high intensity ultrasound surgeries had evolved into clinical use, and they were being used to disintegrate gall bladder stones and break down various tumors in the brain and pancreas.
 |
| A therapeutic ultrasound transducer exerting a force on the surface of water. |
Imaging and surgical techniques use opposite frequencies of sound waves to either provide an image (very high frequency waves) or to break up a mass (very low frequency waves). More recently, in the last 20 years, scientists have found uses for sound waves in the mid-ultrasonic-frequency ranges. Termed “therapeutic ultrasound,” the mid-level ultrasonic waves are utilized to treat tissues directly and enhance the successful outcomes of other treatments.For example, therapeutic ultrasound is used to deliver drugs through the skin without needles, to enhance bone healing and growth, to provide arthritis relief and reduce joint inflammation, and more recently, to enhance drug delivery to brain tissues to aid in the treatment of neurological diseases.
Since the 1960s with the development of the gamma knife, little progress has been made in treating brain cancer, and most forms of treatment are ineffective. Brain cancer continues to be the leading cause of cancer-related death in patients younger than age 35. A critical problem in treating brain cancer is the physician’s inability to remove or destroy all the cancerous tissue and surrounding tissue without causing serious mental impairment to the patient.
Therefore, in many cases, certain cancerous cells escape treatment and grow back stronger. In the last 10 years, recent developments in drug delivery methods have allowed doctors to implant/inject time-release drugs into the tumor location, thereby allowing for continuous release of chemotherapy; however, results from these studies have not been as successful as anticipated. It is believed that the non-treated cancerous cells are able to migrate from the original tumor site, and relocate beyond the range of the injected chemotherapy treatment.
The Targeted Drug Delivery Laboratory at Cornell University has begun to test the technique of using Therapeutic Ultrasound to enhance the success of chemotherapy treatments. Scientists are currently using Therapeutic Ultrasound to increase the distribution of chemical dye agents (mimicking chemotherapy) into mock-tissue “phantoms” that mimic brain tissue. Studies are also being conducted using these techniques on avian and equine tissues. Scientists have found in these tests that the use of Therapeutic Ultrasound enhances the chemotherapy delivery and also reduces the time necessary for the drug to work. Scientists hope to use the same techniques to increase the effectiveness of chemotherapy as well as reduce the time it takes for the drugs to work in a given patient (e.g., to reach the cancerous brain tissue quickly and before the cells can migrate and regenerate).
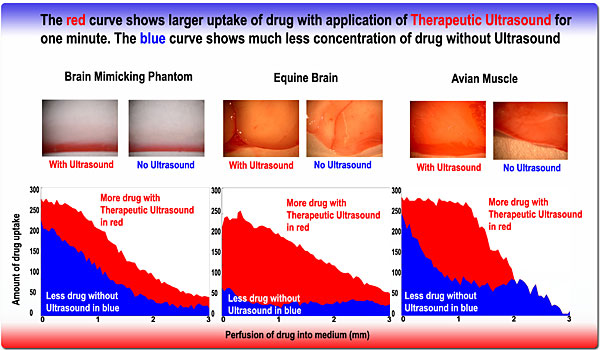
The above Figure shows the results of enhanced drug delivery into a brain mimicking phantom, equine horse brain and avian muscle tissues with the application of Therapeutic Ultrasound for one minute in red, compared with the control in blue. The figure shows that local delivery of drug in conjunction with the application of Therapeutic Ultrasound may significantly enhanced the amount of drug delivery to tissue.
From current research, Cornell scientists conclude that Therapeutic Ultrasound may potentially impact brain cancer treatment, allowing doctors to infuse drugs directly at the tumor site and/or tumor cavity, while simultaneously administering Therapeutic Ultrasound to enhance the movement of the chemotherapy through the tissue. In such cancer drug delivery regimens, enhancing drug uptake into the tissue will undoubtedly play a major role in reducing the recurrence of brain tumors and migratory effects of the cancerous cells, and help prevent cancer from spreading.
George Lewis, one of the scientists conducting the Therapeutic Ultrasound research at Cornell believes that this breakthrough will aid physicians in treating brain cancer. “An analogy is likening the human brain to a damp sponge. If you were to hold the sponge under a dripping faucet, it would slowly absorb more water until it became saturated, “Mr. Lewis said. “However, if you move the sponge and squeeze it in your hand while it is under the water faucet, the sponge would absorb more water and become saturated much more rapidly.” Mr. Lewis said that similarly, ultrasound is a mechanical wave that, when traveling through the brain, creates the same “sponge effect” on chemotherapy, intensifying it and spreading it more effectively.
Mr Lewis explained that the effects of ultrasound energy as it passes through tissue may be manifested in various forms. Heat or warming from the mechanical ultrasonic vibration of cells and molecules has a direct effect on enhancing tissue permeability and diffusion speeds. Local warming of the target tissue (e.g. tumor or resection cavity) below tissue damage may also enhance the movement of drug into the tissue of interest. Along with warming, as acoustic waves propagate, a forward pressure is generated which imparts a direct force upon the tissue (acoustic radiation pressure). “Like an ocean wave hitting a swimmer and throwing him off course, the acoustic pressure wave can put a force on matter and physically change its position” Mr. Lewis commented. In this case of drug delivery, the force can be used to drive chemotherapy further into the tissue. Both warming and acoustic pressure effects can decrease drug delivery time and increase uptake.
The use of therapeutic ultrasound in medicine is about to arrive and holds many possibilities in the near future. From applications in enhanced drug uptake, local treatments of bone and joints, to studies currently being conducted in cosmetic applications and dentistry, ultrasound is no longer used just for imaging. Continuing research at the Targeted Drug Delivery Laboratory of Cornell University and Transducer Engineering, Andover MA will push applications from in vitro studies of phantoms and excised brains into animal brain cancer models to study its effectiveness in human application.
The research for this work was supported in part by the National Science Foundation, the National Institutes of Health, and Transducer Engineering Incorporated.
[ Lay Language Paper Index | Press Room ]