Xinliang Zheng – lzheng@intven.com
Sourabh Kulhare – skulhare@intven.com
Courosh Mehanian — cmehanian@intven.com
Ben Wilson — bwilson@intven.com
Intellectual Ventures Laboratory
14360 SE Eastgate Way
Bellevue, WA 98007, U.S.A.
Zhijie Chen – chenzhijie@mindray.com
SHENZHEN MINDRAY BIO-MEDICAL ELECTRONICS CO., LTD.
Mindray Building, Keji 12th Road South,High-tech Industrial Park,
Nanshan, Shenzhen 518057, P.R. China
Popular version of paper 1aBA5
Presented Monday morning, November 5, 2018
176th ASA Meeting, Minneapolis, MN
A key gap for underserved communities around the world is the lack of clinical laboratories and specialists to analyze samples. But thanks to advances in machine learning, a new generation of ‘smart’ point-of-care diagnostics are filling this gap and, in some cases, even surpassing the effectiveness of specialists at a lower cost.
Take the case of pneumonia. Left untreated, pneumonia can be fatal. The leading cause of death among children under the age of five, pneumonia claims the lives of approximately 2,500 a day – nearly all of them in low-income nations.
To understand why, consider the differences in how the disease is diagnosed in different parts of the world. When a doctor in the U.S. suspects a patient has pneumonia, the patient is usually referred to a highly-trained radiologist, who takes a chest X-ray using an expensive machine to confirm the diagnosis.
Because X-ray machines and radiologists are in short supply across much of sub-Saharan Africa and Asia and the tests themselves are expensive, X-ray diagnosis is simply not an option for the bottom billion. In those settings, if a child shows pneumonia symptoms, a cough and a fever, she is usually treated with antibiotics as a precautionary measure and sent on her way. If, in fact, the child does not have pneumonia, this means she receives unnecessary antibiotics, leaving her untreated for her real illness and putting her health at risk. The widespread overuse of antibiotics also contributes to the buildup in resistance of the so-called “superbug” – a global threat.
In this context, an interdisciplinary team of algorithm developers, software engineers and global health experts at Intellectual Ventures’ Global Good—a Bill and Melinda Gates-backed technology fund that invents for humanitarian impact—considered the possibility of developing a low-cost tool capable of automating pneumonia diagnosis.
The team turned to ultrasound – an affordable, safe, and widely-available technology that can be used to diagnose pneumonia with a comparable level of accuracy to X-ray.
It wouldn’t be easy. To succeed, the device would need to be cost-effective, portable, easy-to-use and able to do the job quickly, accurately and automatically in challenging environments.
Global Good started by building an algorithm to recognize four key features associated with lung conditions in an ultrasound image – pleural line, B-line, consolidation and pleural effusion. This called for convolutional neural networks (CNNs)—a machine learning method well-suited for image classification tasks. The team trained the algorithm by showing it ultrasound images collected from over 70 pediatric and adult patients. The features were annotated on the images by expert sonographers to ensure accuracy.

Figure 1: Pleural line (upper arrow) and a-lines (lower arrow), indication of normal lung
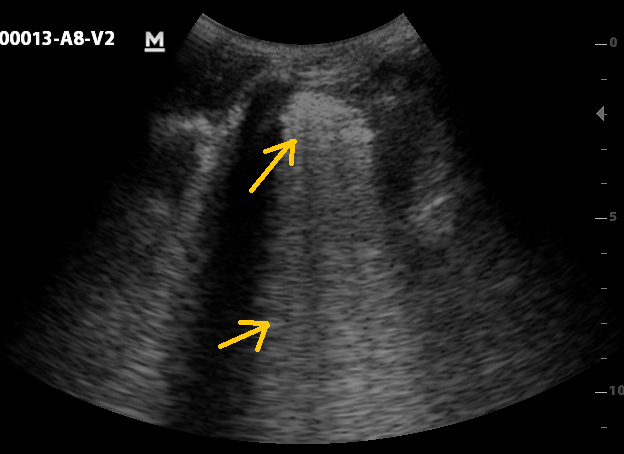
Figure 2: Consolidation (upper arrow) and merged B-line (lower arrow), indication of abnormal lung fluid and potentially pneumonia
Early tests show that the algorithm can successfully recognize abnormal lung features in ultrasound images and those features can be used to diagnose pneumonia as reliably as X-ray imaging—a highly encouraging outcome.
The algorithm will eventually be installed on an ultrasound device and used by minimally-trained healthcare workers to make high-quality diagnosis accessible to children worldwide at the point of care. Global Good hopes that the device will eventually bring benefits to patients in wealthy markets as well, in the form of a lower-cost, higher quality and faster alternative to X-ray.
